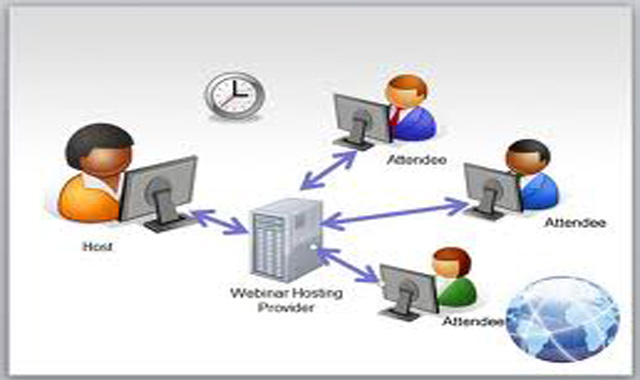
The electronic health record is at the heart of efforts to improve clinical documentation. One effort strives to get disparate EHR software programs—and the physicians using them—to encode problem lists in a common way.
This article appears in the March 2014 issue of HealthLeaders magazine.
With the October 1 activation date for ICD-10-coded payments and the end-of-year move to meaningful use stage 2, this will be a watershed year for clinical documentation improvement.
Technology is playing a big role in both efforts. To an unprecedented degree, and with significant cost and effort, the electronic health record is becoming the heart of clinical documentation improvement—prompting doctors to enter more specific diagnoses, reducing the need for labor-intensive coding, and propagating a common vocabulary between disparate care coordinators to enhance decision support.
“Clinicians are taking care of patients, doing their documentation as they always have, but interface terminology actually gives them phrases or other things that they can use, and those are mapped to SNOMED and often to ICD,” says Rita Scichilone, who until recently was senior advisor for global standards at the American Health Information Management Association.
SNOMED CT—the Systematized Nomenclature of Medicine Clinical Terms—is required to be generated by EHRs in order to be certified under the meaningful use stage 2 program. “SNOMED CT is a terminology, actually the language of medicine, which makes it very different than a classification system” such as ICD-10, Scichilone says.
One of SNOMED CT’s great benefits is it requires disparate EHR software programs—and the physicians using them—to encode problem lists in a common way, Scichilone says. Prior to the SNOMED CT requirement, EHR software supported a variety of encoding schemes, which often made interoperability and sharing of problem lists impractical.
“Clinical quality measures that CMS is developing are leveraging some of the SNOMED vocabularies to define the numerator and the denominator of a particular patient that has a particular kind of diagnosis or condition,” says Doug Fridsma, MD, PhD, chief science officer and director of the office of science and technology in the Office of the National Coordinator for Health Information Technology.
“For example, if somebody has a fractured right leg, SNOMED would have three concepts—a right concept, a leg concept, and a fracture concept—and you’d put all three of those together to create the right leg fracture,” says Fridsma. “ICD-10 will have a right leg fracture and a left leg fracture and a right leg fracture complex, so it has to have unique codes for each one of those things. SNOMED actually is designed a lot more in terms of how doctors and clinicians might think, and so they can kind of take the codes that represent the things that they care about—right leg fracture—click on those concepts, and it automatically then generates those three codes together to represent the diagnosis or whatever is there.
“So SNOMED is tremendously powerful, particularly as you want to think about ways to use the structured information to provide better care. It allows you to do things like clinical decision support,” he says.
“Continuous documentation improvement works with the doctor to advise them to add language to let their diagnosis tell the story,” says Robert Leviton, MD, chief medical information officer and physician advisor at Bronx (N.Y.) Lebanon Hospital Center, a 972-licensed-bed healthcare system.
“CDI allows us to query the doctor about their patient’s condition when they cannot document all of their concerns in the EMR because they are very busy and must see the next patient in their roster of patients,” Leviton says. “We obtain more detailed diagnostic information. We are able to identify the severity of illness and the risk of mortality so that a patient’s assessment, plans of care, and their principle diagnoses can be reported more accurately to impact reporting to regulatory agencies, assist research, and provide specific information to healthcare plans impacting our hospital’s revenue cycle management.”
CDI technology embedded in EMRs is beneficial in that it can provide guidance to achieve diagnostic specificity required by ICD-10 coding, Leviton says.
“Doctors are not coders,” he says. “They know how to care for patients and determine the best diagnoses. We are structuring our ICD-10 solution to have the doctor select a root diagnosis and then also provide coding qualifications to achieve the most accurate diagnosis. If the doctor selects ankle fracture, for example, we will provide coding qualifiers. Is it the left, right, or bilateral ankle? Is there a component of delayed healing, or nonunion healing? What’s the encounter—is it an initial or subsequent one? Each detail adds to the ICD-10 diagnosis meeting the required detail of the coding system,” says Leviton.
As physicians are prompted to answer these questions, EMR software, in the background, picks the codes that best match the physicians’ answers. CDI coding specialists can then refine or ask for even more specificity from physicians to further optimize this coding, Leviton says.
SNOMED coding facilitates sharing of problem lists, procedures, and diagnoses in ways that reduce the differing number of terms physicians use for the same things, says George Hickman, executive vice president and chief information officer of the 734-staffed-bed Albany (N.Y.) Medical Center, an academic health sciences center.
“It gives you a better chance to logically operate on that data in ways that others need to do things of a computing nature with that data,” Hickman says.
Despite this, “the vocabulary that they use to express things is somewhat different than the vocabulary at my place, and, therefore, I have to always have my translation thing turned on inside my own head to figure out the differences. So yeah, all these vocabularies are intended to bring us to something in common in understanding,” Hickman adds.
Hawaii Pacific Health, a nonprofit, four-hospital integrated healthcare provider, still relies upon an extensive physician coding group, but it utilizes tools built into its Epic EHR software to make it as easy as possible for the coding to occur, says Steve Robertson, executive vice president and chief information officer. “There’s an ICD-10 diagnosis calculator where the physician enters the diagnosis, but if [the] ICD-10 terms are not quite specific enough, it’ll prompt the physician to add a little bit more specificity.”
Still, Robertson cautions that such computer-assisted coding technology remains somewhat unproven. “It’s still somewhat new, and all these promises of improved productivity may be a pipe dream, depending on how well your engine has been tuned,” he says. “We have bought a product from Dolbey and it is installed. We’re in the process of doing the tuning, so it’s still too early to say what kind of an impact it will have.”
Other providers are pleased with the latest CDI improvements in the EHR software they are using. “It’s all part of the doctor’s work then, and the note and the description and the work that they’ve done in the earlier part of the documentation builds toward using an electronic and computer-based method, builds toward that final code, rather than the doctor having to initiate a whole separate part of engagement, which is just to do the coding,” says Peter Plantes, MD, CEO of Christus Physician Group, which employs more than 150 physicians and other healthcare providers in family practice, internal medicine, pediatrics, OB-GYN, and other multiple medical and surgical specialties, such as orthopedic trauma and cardiovascular surgery. The group operates more than 70 medical clinics throughout Louisiana and Texas, and provides staffing for several hospital-based programs.
Christus uses athenahealth’s EHR software across its approximately 70 outpatient clinics to generate appropriate SNOMED CT and ICD-10 codes, Plantes says. “It’s much more accepted and much better appreciated than athena’s prior internal tool for coding,” he says. “If we had to do this all by intensive training alone, without the SNOMED tool, then the reliability [of] any individual physician through the manual method of what they used to do with ICD-9 would just not have worked at all. This is a huge step forward, and we are supplementing the tool with education.”
In effect, the technology required to achieve both ICD-10 compliance and meaningful use stage 2 attestation has arrived in time for both to occur in 2014, Plantes says.
“Being in approximately 70 different communities across two states, we need and absolutely require Internet-based clinical solution tools to be able to execute our strategies that are both required by things such as meaningful use as well as what we want to do with advancing our quality program,” he says.
While providers such as Christus are able to rely upon the efforts of vendors such as athenahealth to supply CDI technology, other large providers have different strategies.
Kaiser Permanente had an existing set of clinical terms that were mapped to ICD-9 CM and SNOMED for use in diagnosis and problem list entry. In 2011, the Kaiser Permanente Convergent Medical Terminology team began an effort to transition this set of clinical terms to ICD-10-CM. The effort was referred to as a “graceful transition” based on the strategy to implement the changes in small increments over the course of several years, rather than making one significant change on October 1, 2014. This required that new clinical terms added to production be mapped to both ICD-9-CM and ICD-10-CM.
Initially, Kaiser’s team performed a preliminary evaluation of ICD-10-CM to determine the areas with the most potential impact to end users, according to Moon Hee Lee, director of convergent medical terminology at Kaiser Permanente. The existing set of clinical terms was then divided into logical groups based on medical specialties, such as cardiology. “We began with groups of terms having the least impact to end users, which meant the terms in noninjury categories,” Lee says. “We first mapped the existing terms to ICD-10-CM, and then compared them to the ICD-10-CM code ranges to identify any gaps.”
When Kaiser’s team uncovered gaps, a team of terminology modelers consisting of physicians and nurses reviewed each of the ICD-10-CM codes in the gap to determine what clinical concept was implied by those ICD-10-CM codes. They then created new clinical terms to add to the diagnosis and problem list term set, and mapped them to equivalent SNOMED concepts.
When equivalent SNOMED concepts were not available, the team would model new SNOMED concepts following the SNOMED editorial guidelines. These concepts were then mapped to both ICD-9-CM and ICD-10-CM by two independent coders, Lee says.
“When a group of terms is completed, we determine what would be useful as a problem list subset and then donate that problem list subset to IHTSDO and the National Library of Medicine,” Lee says. IHTSDO, the International Health Terminology Standards Development Organisation, is the Denmark-based not-for-profit association that owns and maintains SNOMED CT.
The subsets donated to date include the Clinician Display Names, as well as associated Patient Display Names, ICD-9-CM mapping, ICD-10-CM mapping, and existing or new SNOMED concepts modeled by Kaiser Permanente.
“As we enter 2014, we have made significant progress in this work and are well-positioned to complete the transition activities ahead of the October 1 implementation date,” Lee says. The progress made to date, she says, is in part due to a strong level of collaboration with the Kaiser Permanente terminology working group, which consists of physician users from seven Kaiser Permanente regions who review the clinical terms created by CMT for end-user usability.
The extent to which Kaiser Permanente has had to blaze trails in CDI points out the tremendous cost that can be incurred—cost often incurred by vendors, but also providers themselves if they develop their own EHR software.
Beth Israel Deaconess Medical Center is one such provider. At the November 13, 2013, meeting of HHS’ Health IT Standards Committee, John Halamka, MD, who is CIO and senior vice president of information systems for the Boston-based 649-bed teaching hospital, revealed that the cost of its clinical documentation improvement project has skyrocketed.
“The regulation originally assessing the impact of ICD-10 suggested that Beth Israel Deaconess should spend $600,000 and would achieve everything that was necessary,” Halamka said. “I’m now $10 million into the project and we’re not quite done yet. It’s not the retrofitting of the financial and the clinical systems to hold an alphanumeric code that’s seven characters long; it’s reengineering the clinical documentation processes to effectively support the code that you have to specify. That’s hard work.
“We’d hoped that SNOMED could inform the ICD-10 selection so that you would link the problem list, the documentation, and the billing into one workflow. And we have yet to see products that really do that.” Source