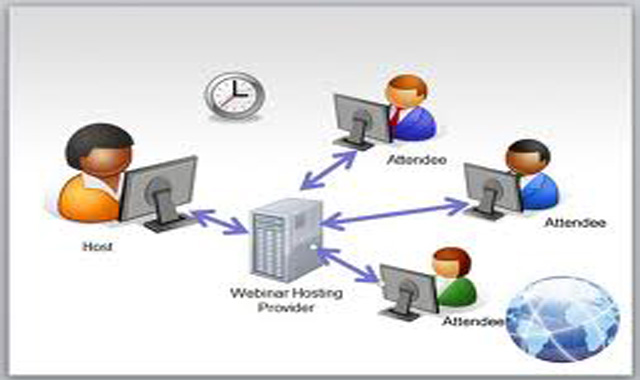
Those interested in understanding and improving the health care system have long used information in medical claims—bills submitted by physicians and hospitals for payment by commercial and government health plans. This information helps health administrators, researchers, and policy makers to understand the cost and quality of health care and identify patients at risk of developing chronic conditions, pinpoint billing fraud, and improve patient care (e.g., by finding patients who are overdue for mammography or other recommended care).
So what is claims data? Claims data consists of the billing codes that physicians, pharmacies, hospitals, and other health care providers submit to payers (e.g., insurance companies, Medicare). This data has the benefit of following a relatively consistent format and of using a standard set of pre-established codes that describe specific diagnoses, procedures, and drugs. Additionally, since all health care providers want to be paid for their services, nearly every encounter that a patient has with the medical system leads to the generation of a claim, creating an abundant
and standardized source of patient information.
More recently, however, a new world of data has become increasingly available for analysis: data from the electronic medical record (EMR). Because the EMR is the software which is accessed directly by physicians to record the details of their encounters with patients, it contains a rich array of data not available elsewhere.
This paper makes the case that neither claims data nor EMR data alone allow for optimal analysis of patient health status, but rather that the best practice of health analysis depends on using both of these data types together.
The advantages of claims data
Before extolling the virtues of EMR data, it should be said that claims data has a lot going for it. Perhaps the main advantage is that it is only through claims data that a holistic view of the patient’s interactions with the health care system can be seen.
Consider, for example, Steve, a patient with diabetes. Steve might have an appointment in March with his primary doctor. Before the appointment, he might stop at a lab affiliated with his doctor’s office to have his cholesterol checked. Then in April, Steve might visit his eye doctor to make sure that diabetes hasn’t affected his vision. Finally, in May he might go to his local pharmacy to refill his insulin prescription.
So how will all of this activity be documented in the EMR? In many cases, only a subset of this activity is recorded within an EMR. This is true because, in spite of federal incentives encouraging EMR adoption, in 2011 only 57 percent of office-based physicians used an EMR.1 So, if Steve’s primary doctor uses an EMR but his eye doctor does not, data from his primary doctor’s EMR may contain no evidence whatsoever that an eye exam was performed. Additionally, while Steve’s doctor may use the EMR to write and print a prescription for Steve’s medications, the EMR system may not be connected to the pharmacy and therefore may not record whether Steve ever filled (or refilled) his prescription. And even when physician offices are electronically connected to pharmacies (36 percent of offices in 2010),2 that connection often allows only the electronic transmission of the prescription to the pharmacy without sending any information back to the physician about whether or not the
prescription was ever filled or refilled.