By Thanh Tran, CEO, Zoeticx and David Conejo, CEO, Rehoboth McKinley Christian Health Care Services
Can healthcare institutes afford not to engage in the 2020 wave of healthcare disruption? While healers are not prognosticators, savvy healthcare CEOs have their eye on 2020. For those riding the disruption wave, the answer is simple. CMS alone is putting out more than 80 billion in reimbursements for preventive care initiatives. This calculation alone does not count on complex chronic care conditions and other follow-ups from preventive care engagements. Private healthcare payees are not far from this evolution as well.
Also, CMS and private healthcare payees have contained the growth of acute care reimbursement. It has almost the same ‘carrot and stick’ model for the evolution from paper to electronic. Continue to use the paper method and you will get penalized. Get on the electronic record train, and you will receive financial incentives.
Earthquake or Hurricane?
Both natural disasters are simply disasters. We do not bring this up from the disaster standpoint, but from our current ability to monitor the progress towards controlling the impact. Earthquakes cannot be foreseen, but hurricanes can.
The paper evolution is like an earthquake to healthcare with its impact still being felt today. There is not much planning upfront. The preventive care evolution is more like an imminent hurricane. We know it is coming, we know approximately when it will land, but we don’t know where it is going. We need to plan to deal with it and manage where it will take us. Those unprepared will suffer the most negative impacts. Will your healthcare institute take this risk?
Most healthcare institutes have deployed an EHR system, almost completing the evolution from paper to electronic medical records. This was the first wave of healthcare disruption. However, we now know that this was much more of a disruptive process in healthcare than anyone realized, as its impact has gone way beyond how patient medical data is recorded.
Power vs. Paper
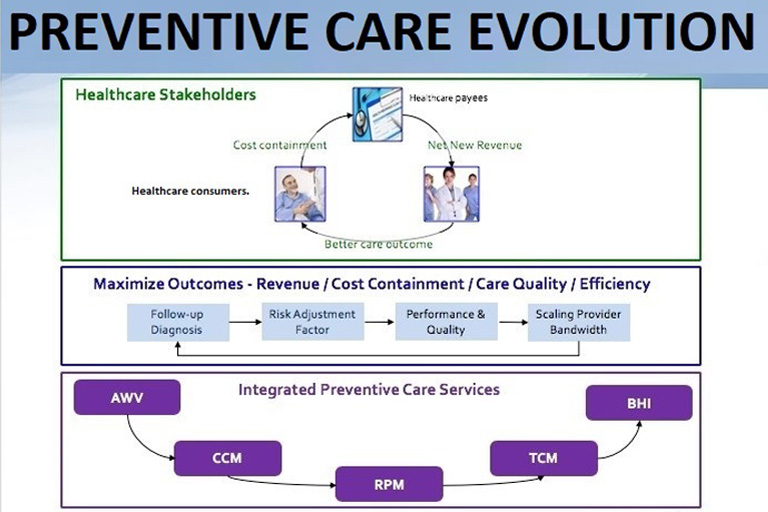
It began with requirements for care providers to use an electronic system in place of a traditional paper approach, creating the potential for patient medical information exchange which will improve care quality and efficiency. CMS rolled out preventive care reimbursements starting with the Annual Wellness Visit (AWV).
CMS then continued to invest in preventive care through additional reimbursements such as Chronic Care Management, Remote Patient Monitoring, Behavioral Health Integration and Transitional Care Management. This strategy is based on the Patient Centered Medical Home (PCMH) with the objective to curb healthcare costs with preventive care measures, a 6:1 ROI versus acute care.
Reimbursements as incentives led to the next wave of healthcare disruption in which care providers’ workflows were impacted on how to record patient medical records. These preventive care initiatives created fundamental changes impacting almost every operational aspect of a care provider’s workflow.
Preventive Care
Today, it is all about preventive care: simply put, the patient is not yet a patient until he or she encounters pain. The patient is not yet sick. The operational model is not reactive. The demand is to anticipate and monitor conditions so care providers can act before the patient encounters a serious medical problem. This causes changes in the operational workflows for healthcare institutes and their workflow. In the patient engagement model, there is the acute care model, it is the patient who makes an appointment or visit. For preventive care, it is care providers and healthcare institutes conducting the outreach. However, without the patient outreach model, healthcare institutes cannot realize the full financial incentives offered by CMS.
In non-face-to-face engagements, patients contact their primary care providers for consultation, but that non-face-to-face model is different from the preventive care one. In the acute care environment, care providers cannot bill for the engagements, it is visits and appointments. In the preventive care environment, care providers can bill for the services, but it is up to the care providers (and their staff) to reach out and monitor patient conditions.
Then there is the question of scalable bandwidth. In an acute care environment, the patient’s coverage is limited to the traditional eight-hour shift. In this case, simple math indicates that the number of patients an office can handle per day is based on the time a physician could spend with the patient. That model does not work in a preventive care environment because the number of patients is not based on their sickness, but the population of patients with a specific set of conditions. Physicians need to delegate more to the clinical staff, extending its bandwidth beyond the working hour.
Resources must also be planned for. The acute care model starts with a receptionist greeting the patient, front office checking for insurance eligibility, then the nursing staff performs vital measurements, the physician encounters the patient and ends with billing for encounters. The critical resource limiting the scalability of that operation has been the physician at the center.
Physicians establish the boundary of patient monitoring activity and clinical staff takes the major roles in reaching out, monitoring patient conditions and only escalates to the physician on concerned events. Care resource planning becomes the critical component for preventive care services, requiring how to scale for the care providers’ bandwidth.
Effective Billing
Billing is not by visit or appointment but based on time monitored. The amount of billing is based on how effective your system is in reminding you to reach out and maximize your clinical staff bandwidth for such activities.
Healthcare IT is transforming from the necessary evil to the savior of the day. Today workflow is either manual or passive, based on an event initiated by the patient. In the preventive care model, as the ratio of patient to care providers increases, the demand for workflow automation increases.
It begins with a reminder, then tracking to the overall collaboration among care providers. EHR is the necessary evil in the room mandated by the ACA. The next wave of healthcare IT solutions will be the savior for care providers to maximize their revenue from preventive care. And yes, it is an indirect “must have” as healthcare payees are focusing more on preventive care.
2020–Beyond healthcare IT
Healthcare IT is the enabler of preventive care delivery, but preventive care delivery requires more than the enabler. Look at a simple case of Remote Patient Monitoring in which data is collected from medical devices. Medical devices are used by patients. If patients do not use the medical devices, there is no data to collect, no data analysis and therefore no monitoring.
But let’s investigate it a tiny bit closer. Patients are required to ‘operate’ the medical devices. Clinical staff is expected to help patients set up monitoring environments consisting of medical devices. If patients encounter issues with the medical devices, they are expected to call someone – that someone is a consumer support organization for that product.
Either nursing staff will be expected to be a lot more IT savvy or another support component with some fundamental healthcare knowledge will provide patient support. Healthcare IT can ease the data flow, ease the user experience, ensure secure data flow, but the operational model is required to inject more components in the workflow.
So, as we begin to turn the calendar page to 2020, it is important that healthcare institutes prepare and not be disrupted.